Join Our eNewsletter!
Subscribe to our monthly newsletter to receive encouraging advice to help you lead a healthy lifestyle.

Good Bones: Start Early to Prevent Osteoporosis
By Christina Frome, MD, FACOG
Osteoporosis is a condition that causes bones to become porous, weak, and brittle. It’s an invisible disease with no obvious signs or symptoms until a bone breaks. One in three women 50 and over will experience a fracture due to osteoporosis. And contrary to the common belief that the disease only affects women, one in five men will also suffer an osteoporotic fracture.
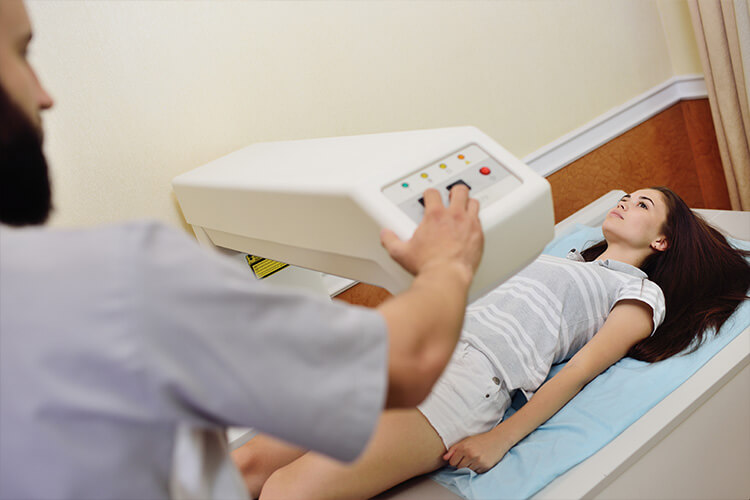
A DEXA scan is recommended for all women over 65 and all men over 70, as well as women between the age of 50 and 65 who are at higher risk for osteoporosis. It’s a simple, 15-minute test repeated every two to five years that takes radiographic images of the body to determine bone density. The result of the test is a T-score, which compares bone density with that of a healthy 30-year-old. A T-score of -1.0 to -2.5 signifies low bone density, which is a precursor to osteoporosis. Below -2.5 translates into more than 25% bone loss, which is considered full-blown osteoporosis.
Osteoporosis is painless, but the possible consequences of it aren’t. Bone fractures can happen very easily from a fall or even simply bumping into something. The most common fractures are of the wrist, upper arm, shoulder, pelvis, hip, and spine. And a person who has suffered one osteoporotic fracture is twice as likely to suffer more fractures in the future. One in four women who have had a spine fracture will sustain another fracture within a year. The chronic pain and immobility caused by these fractures can lead to a loss of independence and decreased quality of life. And more than 20% of people who have hip fractures will die within the first year of the fracture. The good news is that for many people, osteoporosis is preventable – if you take measures early enough.
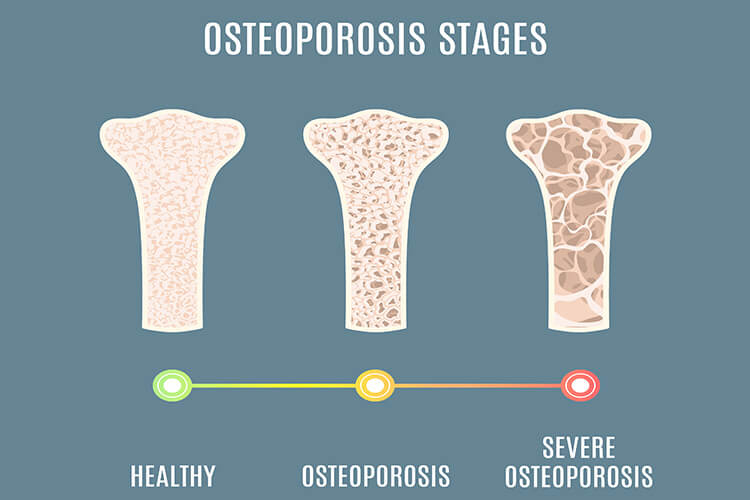
What Causes Osteoporosis?
When we’re young, our bones constantly renew with old bone broken down and new bone generated, which increases our bone mass. As early as our 20s, this process slows and by our 30s, our bone mass peaks. From then on, most of us lose bone mass faster than our bodies create it, which is why people over 50 are at the highest risk. But not all of us develop osteoporosis. If your body built up enough bone mass when you were younger, you’re less likely to develop it.
Unfortunately, there are some uncontrollable factors, other than age, that can make you more susceptible to losing bone mass, including:
- Sex – Women are four times more likely than men to get the disease, due to women having overall less bone mass. Menopause also contributes to the higher risk because when estrogen decreases, osteoclasts, which are cells that break down bones, increase.
- Race – Caucasians and Asians are more likely to develop the disease than other races and ethnicities.
- Small body frame – People with smaller skeletons may have less bone mass to draw from as they age.
- Family history – People who have a parent with osteoporosis or a parent who has had frequent broken bones are more likely to develop the condition.
- Other medical conditions and medications – Certain conditions and the medications taken for them can increase the risk of osteoporosis, including rheumatoid arthritis, Crohn’s disease, chronic kidney disease, HIV/AIDS, hormonal imbalance (low estrogen in women and low testosterone in men), diabetes, and thyroid disease. Other medications can also contribute, such as steroid, some immunosuppressants, certain antipsychotics, anticonvulsants or antiepileptics, lithium, and proton pump inhibitors.
Other Risk Factors
There are some factors that you can control – or at least manage to some degree – to help prevent the development of osteoporosis and the fractures associated with it.
- Smoking – People who smoke or have smoked in the past are at higher risk for osteoporosis and fractures. They’re almost twice as likely to experience a hip fracture.
- Excessive drinking – Consuming more than two alcoholic beverages per day can increase the risk of osteoporotic fractures by 40%.
- Poor nutrition – Not getting enough calcium, protein, fruits, and vegetables can weaken both bones and muscles. Malnutrition in people older than 60 makes them more susceptible to falls and fractures.
- Vitamin D deficiency – Vitamin D is essential to bone health, and it helps our bodies absorb calcium, so a deficiency makes osteoporosis and fractures much more likely.
- Not getting enough calcium – People who have a lifelong lack of calcium in their diet, or who have trouble absorbing calcium, tend to experience early bone loss, diminished bone density, and more fractures.
- Eating disorders – Anorexia and bulimia can result in being extremely underweight, a dramatic decrease in calcium, and estrogen deficiency, all of which significantly increase the chances of developing osteoporosis.
- Not being active – Exercise isn’t just for weight loss and increasing muscle. It also helps maintain bone mass. Being sedentary causes bone mass to be lost more rapidly.
- Being underweight – Having a body mass index under 19 increases the risk of osteoporosis, possibly due to underweight people having a small body frame or not getting proper nutrition.
- Frequent falls – 90% of hip fractures happen as a result of a fall. Frequent falling can be due to balance problems, lack of muscle mass, and other issues.
Steps to Prevent Osteoporosis
If you’re over 65 and have had a bone density screening that shows limited bone loss or if you’re under 50, there’s still time to prevent osteoporosis from developing. If you already have low bone density or even osteoporosis, you can’t reverse any bone damage that’s already been done, but you can slow the progression of the disease.

- Stop smoking. Ask your doctor for help quitting if you don’t think you can quit on your own.
- Cut down on alcohol. Limit your alcohol consumption to no more than one drink a day for women and two drinks a day for men.
- Get more Vitamin D. Whenever possible, spend 20 to 30 minutes per day outside (with sunscreen, of course) or take Vitamin D supplements.
- Exercise regularly. Include weight-bearing activities, such as walking, golf, or tennis, as well as strength training exercises. Add in stretching and yoga to improve balance. Avoid high-impact exercises if you’ve already lost bone mass. Always consult your doctor before beginning any exercise program.
- Eat a bone-healthy diet. Focus on foods that provide Vitamin D and calcium, such as dairy, leafy greens, salmon, almonds, eggs, mushrooms, grapefruit juice, and orange juice.
- Achieve a healthy weight. If you’re underweight, do you what you can to gain weight and muscle mass. If you’re suffering from an eating disorder, seek medical attention as soon as possible. On the other hand, being overweight can put excess pressure on your bones, so losing weight, if needed, can also be beneficial.
- Fall-proof your home. If you’re prone to falls because of another medical condition, there may not be much you can do about it. But you can make modifications to your home to help prevent falls. Eliminate slippery rugs and stairs, don’t walk around in socks, add grab bars to the shower, and keep a light by your bed and in your restroom in case you need to get up during the night.
If you’re a woman over 65, a man over 70, or you’re at high risk for osteoporosis, ask your doctor about getting a DEXA bone density scan to determine your likelihood of developing the condition.



